The COVID-19 pandemic has swept the nation, leaving a large portion of the U.S. population infected and undergoing long recovery times. Hospitals in South Georgia are working double-time to try to treat and care for those who are infected. Here are patient testimonials from some of those hospitals.
Chelsie Turrubiartez, 23
Diagnosed: April 5
Hospital: Tift Regional Medical Center/ UFHealth-Shands
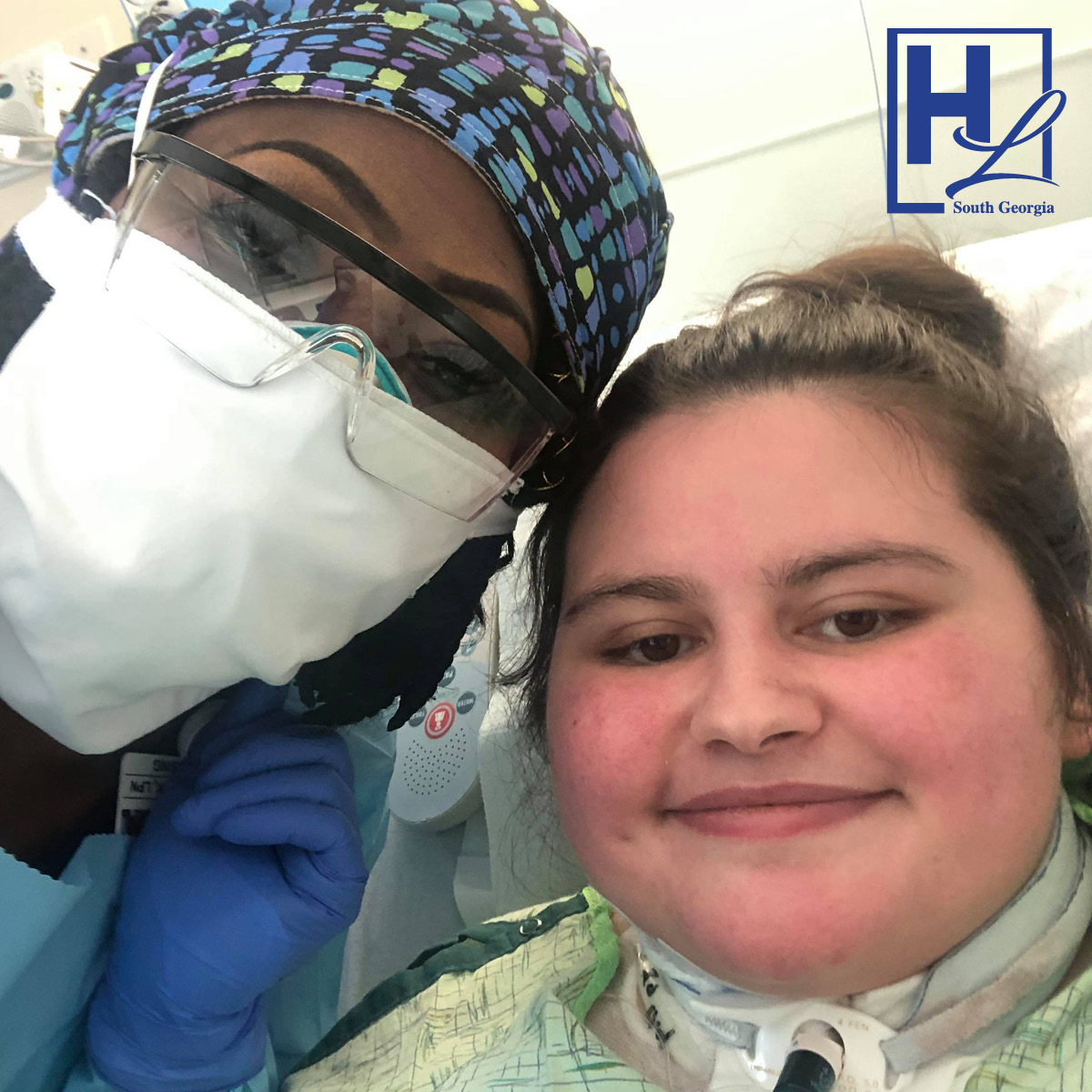
Chelsie Turrubiartez, who works as a nurse at Tift Regional Medical Center, suffered through COVID-19 symptoms for nearly two months. What began as a horrible headache and body aches on March 25 soon progressed to a productive cough, fever, chills, losing sense of taste and appetite, and shortness of breath.
“During all of this, I went through a drive-thru testing at where I work, and they tested me for COVID-19 and the flu,” Turrubiartez said. “My flu test came back negative, and a couple days later I received a call saying that my COVID-19 test also came back negative, and I was relieved.”
After several days with no symptom relief, Turrubiartez decided to call the COVID-19 hotline and was told to get re-tested after describing her symptoms. She went to a clinic, and they took her temperature and checked her oxygen levels where they found them to be in the low 80s. She was then advised to go to the emergency room.“I was immediately placed on a non-rebreather that helped get my oxygen levels up to normal levels again,” Turrubiartez said. “It was believed that I did have coronavirus, and they found that I had pneumonia.”
Turrubiartez was admitted to the ICU and was tested again for COVID-19, but the test still came back negative even though all her symptoms pointed to the virus. On April 1, Turrubiartez said that she was experiencing high levels of anxiety due to her difficulty in breathing properly. Luckily, she had a respiratory therapist she knew from work to stay and help her.
“It was decided that I would be intubated, something I did not want and something I was very terrified of because there was always the possibility that I would not come off of it alive,” Turrubiartez said. “During that time, I begged to the respiratory staff to not let me die. I was sedated and paralyzed and intubated.”
Turrubiartez said that she had good and bad nights after that, but it was decided that she needed to be transferred to another hospital that had the capability and equipment for ECMO (an artificial or mechanical lung of sorts). She was transferred on April 4 to UFHealth-Shands in Gainsville, Florida, and she was officially diagnosed with COVID-19 the next day.
From then on, it was a battle of wills and treatments for Turrubiartez. She had bronchoscopy to help her lungs and a nasogastric tube to help her receive nutrition and oral medications. She said that her medications at both hospitals consisted of antibiotics, heparin, steroids, paralyzing drugs, sedation medication, hydroxychloroquine, and was even accepted to try a trial drug known as sarilumab.
“I was weaned off of ECMO and was taken off on April 21 due to my numbers staying stable,” she said. “On this same day, a tracheostomy was put in due to a person not being able to stay intubated for more than 14 days because of the damage it could cause. I was given convalescent plasma around this time, which is plasma that comes from a person who has the coronavirus antibodies and is recovered and is given to others in the hope that it will help the person’s body fight off the virus.”
On April 24, Turrubiartez was finally deemed stable enough to return back to her hospital in Tifton, Georgia. She was then weaned off of ventilation and kept on medications that helped her stay calm.
“I was kept in isolation, which was the worst part of all of this to me,” Turrubiartez said. “My mom finally was able to drop my phone off, and I was able to communicate with my friends and family,, but it was difficult because I had to work out the muscles in my fingers due to not really using them for so long.”
She started physical therapy soon after, which she said was a challenge because she had to retrain her muscles after not using them for so long.
“Even though it was tough and wore me out, it was my favorite part of the day because I had the best physical therapists that motivated me,” she said. “Eventually, I became strong enough that I was able to walk with a walker. My body had been through so much, but working with physical therapy helped me feel more human, and I was finally able to do more for myself.”
Turrubiartez was tested two more times for the virus, and both tests came back negative. She was then able to be transferred out of the ICU on May 2 and to the medical floor she used to worked on, Medical West.
“I had won one of the hardest battles of my life,” Turrubiartez said. “To this day, I still feel the after effects of going through this ordeal. I was lucky that I have an amazing support system that whenever I feel down or have a breakdown I could call someone and they would answer me and calm me down.”
Martha (Marti) Baker, 67
Diagnosed: March 31
Hospital: Colquitt Regional Medical Center

Marti Baker, who works as a para professional at Colquitt County High School, said that she doesn’t remember most of her COVID-19 experiences because of the severity of her symptoms and the treatments she had to endure. She began noticing symptoms around March 15 with chills and a low-grade fever. By the next week, she was experiencing body aches and had a temperature of 102.4.
“I thought I probably had the flu, so my husband took me to a walk-in clinic,” Baker said. “The nurses at the clinic came to my vehicle to check my temperature and oxygen level and also did the swab for flu, which was negative.”
At this point she was beginning to have shortness of breath, and Baker was sent to Colquitt Regional Medical center to be tested for COVID-19. While waiting for the results, Baker then developed a cough. On March 27, her symptoms took another turn, and she was having nausea and diarrhea. She, along with her husband, took another trip to the emergency room.
“At the ER I was tested for flu again, and this time it showed positive for Influenza Type B, and a chest x-ray showed that I had pneumonia,” she said. “I was released to go home with the usual instructions for flu. The next day I was feeling worse and felt that I was dehydrated. We decided I probably needed some fluids, so we made another trip to the ER.”
The staff at Colquitt Regional quickly stepped up and took Baker into the hospital in a wheelchair while her husband parked the car.
“As he went to park the vehicle, he had no idea that it would be three weeks before he would see me again,” Baker said. “By the time he got back to the ER, they had taken me to a room, and no visitors were allowed.”
Baker said that she wasn’t sure if she passed out or was given medication, but she does not remember her time in the ER from that point onward.
“The only thing I remember from the ER was when I heard someone say that they would have to admit me to the hospital,” she said.
That same night Baker was admitted to the ICU and placed on a ventilator. Her husband was not allowed to visit her, but she discovered after her recovery that he called at least four times a day to check on her. It was on March 31 that they informed her husband that she had indeed tested positive for COVID-19.
Baker was taken off the ventilator two weeks later on April 11. During this time, she has no memory of being taken off the vent. Along with her husband, Baker said that she couldn’t have gotten through this ordeal without the staff at Colquitt Regional.
“I received exceptional care at Colquitt Regional Medical Center,” Baker said. “I didn’t know what was going on with me during the first two weeks there, but I know from talking to my husband that they were taking very good care of me.”
Baker spent the next few days in the hospital, in a regular room, and was finally able to be discharged April 17. As she was getting ready to leave, some of the staff that worked with her came to see her off. That was when she was informed that she was the first COVID-19 patient at that hospital to be taken off the ventilator and discharged to go home.
“I have been totally surprised at how long it takes to recover from this virus,” Baker said. “I have done some research and found that just recovering from the virus can take several weeks, and being on a ventilator and in ICU adds more recovery time.”
On May 25, Baker said she was finally able to stay up all day without needing to lie down and rest. She said that hopefully this was an indicator that she was finally nearing the end of “this terrible journey called COVID-19.”
Her husband, fortunately, never contracted the virus from his wife.
Written by: Alex Dunn
Photography courtesy of Chelsie Turrubiartez and Martha Baker
